A heart attack is a condition that can happen to anybody at any time; unfortunately, pregnant women are no exception. A heart attack during pregnancy is among the most challenging medical conditions.
Although most CPR procedures for a pregnant woman are the same as the standard adult resuscitation, various aspects and concerns are different.
This post will provide you with up-to-date guidelines, information, and recommendations for performing maternal resuscitation.
Heart health and the changes during pregnancy, you need to know

During pregnancy, several anatomies and physiological changes can add an extra strain on the woman’s body, which can sometimes, though rarely, cause cardiac arrest.
Because of the mother and the fetus’s conjoined circulatory system, there is a need for increased blood circulation in the mother’s body.
Due to increased stroke volume and maternal heart rate (15-20bpm), cardiac output rises from 30% to 50%.
Additionally, systemic vascular resistance also decreases due to increased endogenous vasodilators like estrogen, progesterone, and nitric acid, causing a decrease in mean arterial pressure.
Furthermore, the enlarged uterus can produce an afterload increase through compression of the aorta and reduced cardiac return through the compression of inferior vena cava from 12 to 14 weeks of pregnancy.
Due to the increased afterload, the supine position, which is the most ideal for resuscitation, may lead to hypotension.
These physiological, anatomical and pathological changes can make it hard to maintain a clear airway and carry out the CPR process. These challenges can be increased by obesity.
All the experts directly or indirectly involved with obstetric care should be trained and updated on maternal resuscitation methods and considerations.
Common difficulties in pregnant women
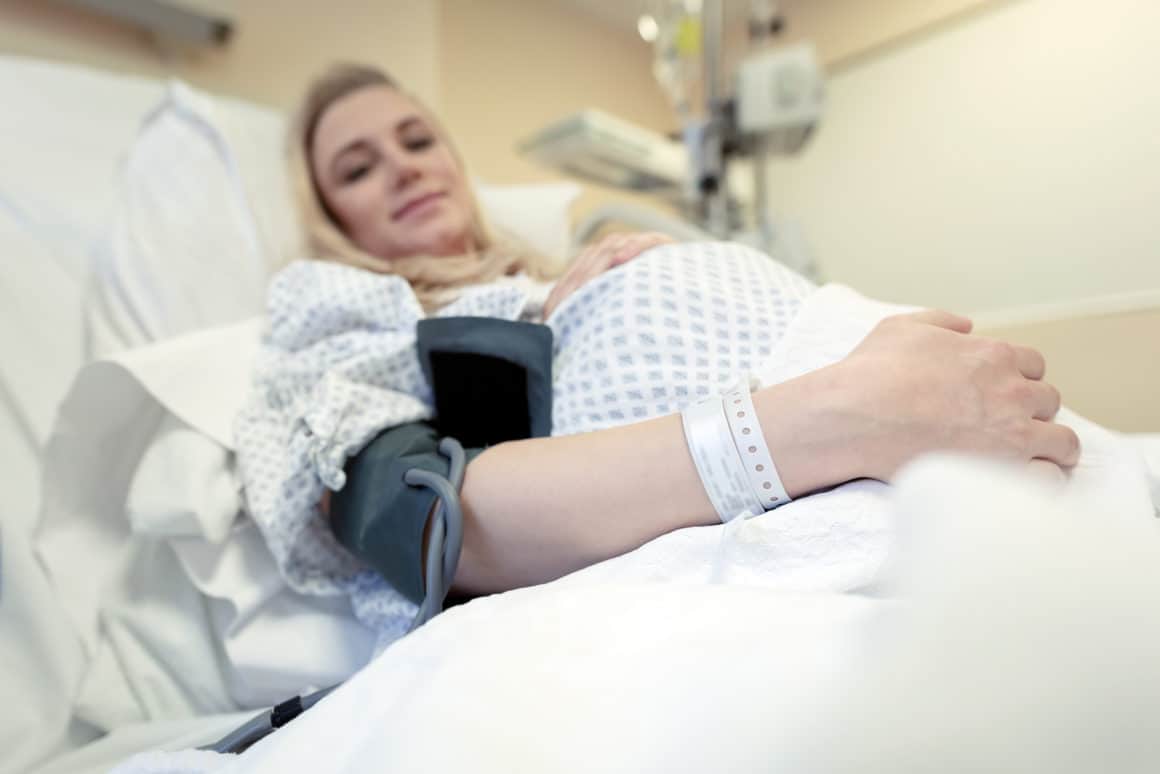
Breathing
- More oxygen requirement.
- Risk of aspiration and regurgitation.
- Difficult to see the rise and fall of the chest when compressing.
- Poor chest compliance.
Airway
Victims should be positioned laterally for the following reasons;
- Inserting airway.
- Suction and aspirations.
- Removal of foreign bodies and dentures.
Circulation
Performing chest compressions is difficult during pregnancy because of the following;
- Raised diaphragm.
- Breasts enlarged.
- Ribs flared.
- Patient obese.
- The supine posture causes inferior vena cava compressions.
Can CPR be conducted on a pregnant woman?
Fortunately, the answer to this worrying question is yes. CPR can be conducted on a pregnant victim. However, a quick response is essential.
Once cardiac arrest or attack is diagnosed, the victim should be laid in an appropriate position, and the basic life support procedure is started immediately. This should continue until the venous access is complete, any causative factors controlled, and emergency medical services arrive.
Basic Life Support procedure

Airway
Quickly establish a clear airway with the head tilt-jaw thrust or head-tilt chin-lift control, then maintained in a fixed position. Use suction to evoke vomit and remove any foreign bodies and poorly fitting dentures and insert the airway.
Carry out the outlined procedure with the patient placed on the supine or laterally inclined with the uterus displaced appropriately.
Breathing
If the victim has stopped breathing properly, start intermittent positive pressure ventilation (IPPV) straightaway once the airway is cleared.
Mouth-to airway, mouth-to-mouth, or mouth-to-nose ventilation should be performed until a self-inflating bag and masks are availed. Continue the ventilation with a reservoir bag and 100% oxygen.
Perform the mouth-to-mouth procedure cautiously to avoid passing oral STI infections if the victim or rescuer is positive for sexually transmitted diseases.
Due to an increased risk of regurgitation and pulmonary aspiration during pregnancy, cricoid pressure or Sellick maneuver should be conducted until the airway is protected with a cuffed tracheal tube.
Keen observation of the rise and fall of the chest is vital as ventilation is made difficult due to reduced chest compliance and increased oxygen requirement. The reduced chest compliance results from rib flaring and splinting of the diaphragm because of the gravid uterus.
Circulation
Circulation problems are diagnosed by the lack of palpable pulse in the large artery. Though chest compressions on the pregnant victim are made challenging by the flared ribs, obesity, and raised diaphragm, it should be performed at the rate or ratio of 15:2.
Due to breast hypertrophy and raised diaphragm, hand position during chest compressions should be moved up the sternum.
The compression of the inferior vena cava by the gravid uterus in the supine position hinders venous return and decreases cardiac output. Unless the compressions are relieved, every attempt to resuscitate will be futile.
Improve venous return and increase cardiac output, place the victim in an inclined lateral position. Raising their legs will also help speed up cardiac output.
Lateral displacement of the uterus
Effective chest compressions can be achieved with patients incline at 30 degrees. However, pregnant patients are prone to roll over when inclined at angles more than this making it hard to perform chest compressions.
Since the Cardiff resuscitation wedge is not available commercially, the use of manual methods is recommended. For instance, the “human wedge” where the victim is inclined on the rescuer’s knees for a stable basic life support position.
Alternatively, upturned chairs and purpose-made wedges in the maternity wards can be used together with pillows and cushions for a soft and stable position for basic life support.
Conclusion
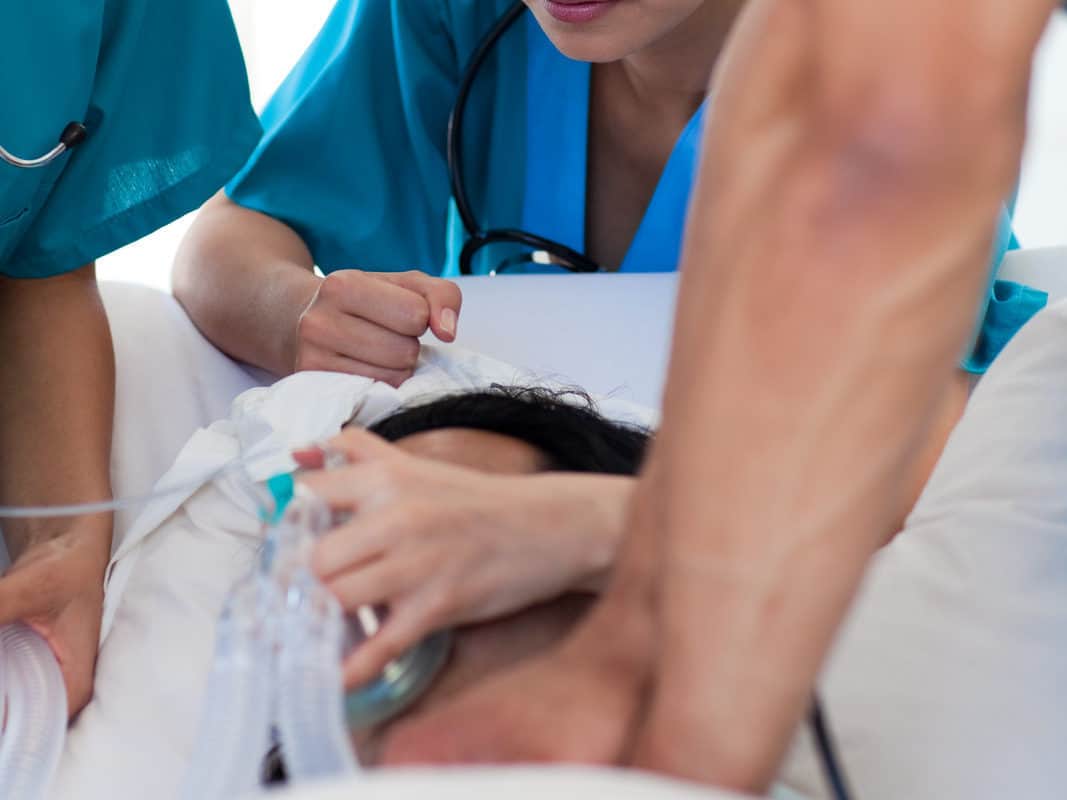
Though performing CPR on a pregnant woman is challenging, it is possible. During pregnancy, CPR’s main aim is to stabilize the mother for a conducive scenario for the fetus.
Immediate response in case of a heart attack is essential despite the various considerations of performing CPR on pregnant victims.
Due to the problems related to resuscitation during pregnancy, members of the public and the emergency service staff should be taken to regular short studies and practice of the basic life support on a manikin.
Training of emergency services staff should be a priority as they are likely the first responders to various obstetric emergency calls.
Finally, when you observe a maternal heart attack victim, call 911, lay the victim on her back, open the airway and confirm if there is no breathing. Start the CPR process until the paramedics arrive.


What pregnant women should know about heart attack risks?
Do only healthy women fall pregnant?